Stroke
Download Video Transcript – PDF Format
Overview
Stroke is the #1 cause of chronic disability and #3 cause of death in Hawaii (State of Hawaii Department of Health, 2017). In 2018, 2.9% of the population of Hawaiʻi indicated they had been told by a doctor, nurse, or other health professional that they had a stroke, which is lower than the national average of 3.4% (Center for Disease Control and Prevention, 2015). However, Hawaiʻi’s rate of stroke mortality is 70.3 per 100,000 people, which is higher than the national average of 58.1 per 100,000 (Centers for Disease Control, 2015). The effects of stroke vary from person to person based on the type, severity, location, and number of strokes. When an area of the brain is damaged from a stroke, the loss of normal function of part of the body may occur. This may result in a disability. Effects of Stroke can impair any or all functions related to speech and language, movement, sensation, eating, swallowing, inability to walk, dizziness, headache, coma, and paralysis.
Stroke Facts
What is a Stroke?
Stroke is caused by blockage of blood flow to the brain, usually due to a blood clot that is lodged within one of the blood vessels to the brain.
For every minute blood flow to the brain is blocked, 1.9 million brain cells die. This is the equivalent of your brain aging 3 weeks per minute, or 3.6 years per hour!
Types of Stroke
- Ischemic Stroke occurs when a blood vessel supplying blood to the brain is obstructed.
- Transient Ischemic Attack (TIA) is a short-term clot or blockage in the brain.
- Hemorrhagic Stroke occurs when a weakened vessel ruptures and bleeds into the brain.
How many people have a Stroke in Hawaii?
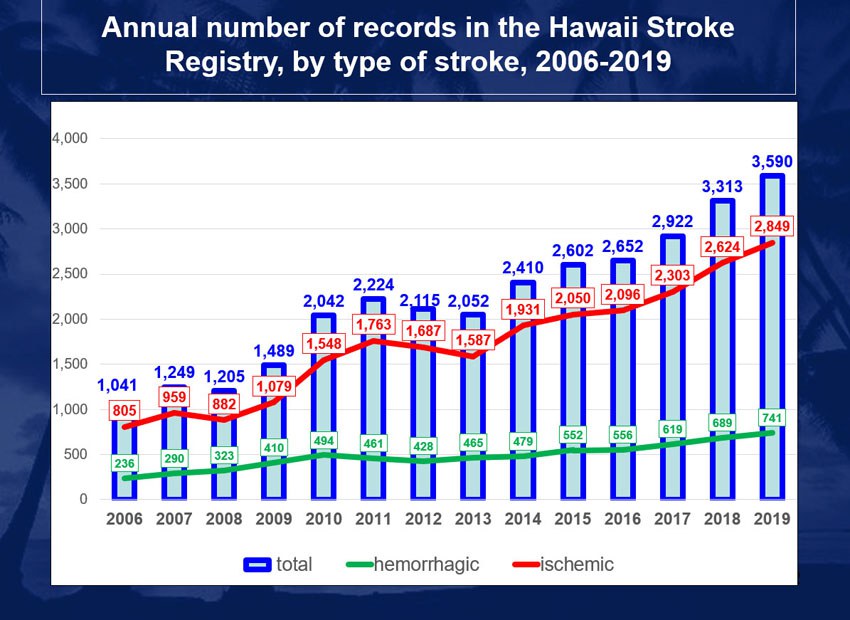
From 2017 to 2019, there was an annual average of 3,275 strokes. 2,592 where ischemic and 683 were hemorrhagic.
Figure 1: Annual Number of Records in the Hawaii Stroke Registry, by Type of Stroke, 2006-2019. Please note that the data in Figure 1 do not indicate an increasing number of strokes, but rather an increasing number of hospitals contributing data to the Hawaii Stroke Registry.
Annual number of records in the Hawaii Stroke Registry Long Description
Risk Factors of Stroke
Medical Conditions
- High Blood Pressure
- High Blood Cholesterol
- Heart Disease
- Diabetes
- Overweight and Obesity
- Sickle Cell Disease
- Previous Stroke or Transient Ischemic Attack (TIA)
If you’ve already had a stroke or a TIA, there is a high probability you could have a stroke in the future.
Behaviors
Risk Factors Not Within Your Control
- Age
- Family History
- Race
- Gender
Stroke Prevention Tips
The American Association Life’s Simple 7®
- Stop Smoking – Learn How to Stop Smoking
- Eat Better – Learn How to Eat Better
- Get Active – Learn How to Get Active
- Lose Weight – Learn How to Lose Weight
- Manage Blood Pressure – Learn How to Manage Blood Pressure
- Control Cholesterol – Learn How to Control Cholesterol
- Reduce Blood Sugar – Learn how to Reduce Blood Sugar
Other Prevention Tips
- Limit alcohol use.
- Take your medicine to treat high cholesterol, high blood pressure, or diabetes as directed.
- Talk with your health care provider about a plan to treat the medical conditions that may lead to stroke.
Stroke Symptoms
Call 911 if these signs are present:

Be Fast for Stroke Poster – PDF Format
| NUMBNESS | or weakness of face, arm, or leg, especially on one side of the body. |
|---|---|
| CONFUSION | trouble speaking or understanding speech. |
| TROUBLE SEEING | in one or both eyes. |
| TROUBLE WALKING | dizziness, loss of balance or coordination. |
| SEVERE HEADACHE | with no known cause. |
If You Have a Stroke
When to Seek Immediate Medical Attention
If you or someone near you is experiencing stroke symptoms, act F.A.S.T. and call 911 to seek treatment immediately. Stroke treatments that work best are available only if the stroke is recognized and diagnosed with 3-4.5 hours of the first symptoms. Stroke patients may not be eligible for these treatments if they do not arrive at the hospital in time. If you’re able to, note the time when any symptoms appear.
This information helps health care providers determine the best treatment for each person. Do not drive to the hospital or let someone else drive you. Call an ambulance so that medical personnel can begin life-saving treatment on the way to the emergency room.
Stroke Treatment
Treatment begins when the emergency medical services (EMS) arrives to take you to the hospital. Upon your arrival, you may receive emergency care, treatment to prevent another stroke, rehabilitation to treat the side effects of stroke, or all three.
On the Way to the Hospital
- If someone you know shows signs of stroke, call 9-1-1 right away.
- Do not drive to the hospital or let someone else drive you.
- Key to treatment and recovery is getting to the hospital quickly.
- Calling an ambulance means that medical staff can begin life-saving treatment on the way to the hospital. Stroke patients taken to the hospital in an ambulance may get diagnosed and treated more quickly than those who do not arrive in an ambulance.
- Emergency workers can take you to a specialized stroke center to ensure that you receive the quickest possible diagnosis and treatment. Emergency workers will also collect valuable information that supports treatment and will alert hospital staff before you arrive, giving them time to prepare.