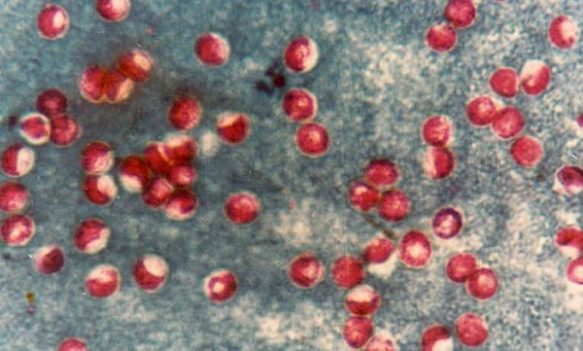
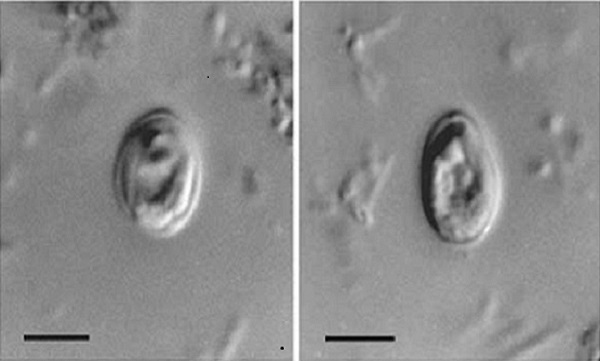
Cryptosporidiosis
Report a Case
Disease Reporting Line:
(808) 586-4586
Signs and Symptoms
The symptoms usually start about 7 days after exposure to the parasite, but they can begin from 1 to 12 days after exposure. The major symptoms are stomach cramping and frequent, watery diarrhea. Less commonly, nausea, vomiting, and fever may also occur. Symptoms may last for several days to several weeks, but should resolve within one month for healthy individuals.
Transmission
Cryptosporidiosis is spread by eating food or drinking water contaminated with stool from infected animals or humans. The disease can be spread person-to-person, animal-to-person, and by contaminated food.
It is commonly spread through swimming pools, since the parasite has a high tolerance for chlorine, it can survive in maintained pool systems. Avoid drinking pool water. Cryptosporidium eggs can stay alive outside the body for 2 to 6 months in moist settings.
Diagnosis
Cryptosporidium cannot be detected with routine stool cultures. Your doctor must order a special stool test that can detect parasites.
Treatment
The illness usually passes in 3 to 7 days in most people; however, doctors can also prescribe anti-parasitic medications for severe illness or to shorten duration. Persons with this illness should drink plenty of fluids to replace what is lost in diarrhea. The infection can be serious, even life threatening, when it occurs in persons whose immune systems are weakened by certain medical treatments or diseases such as cancer or HIV/AIDS.
Risk in Hawaiʻi
Cryptosporidiosis is present in Hawaii, but it is uncommon. Many cases are linked to travel to other states or countries.
Prevention
Any child with diarrhea should stay from day care until the diarrhea stops. Also, people with diarrhea who work in food-handling or take direct care of patients should stay home from work until well. Infected people with no symptoms who work as food handlers, childcare and health care workers, should get permission from their doctor or the Health Department before returning to work. A person with cryptosporidiosis may be able to spread the disease for several weeks after the symptoms have gone away. Therefore, careful hand washing is very important upon return to work.
- Wash your hands carefully after using the toilet, after changing diapers, after handling animals, and before eating or making food. After changing diapers, wash the child’s hands as well.
- Dispose of human and animal waste promptly and carefully.
- Avoid drinking untreated water from ponds, lakes, streams, swimming pools, hot tubs or fountains. If you must drink untreated water, first bring it to a rolling boil for at least 1 minute.
- Cryptosporidium can live for days in swimming pools even with proper chlorine levels. Always shower before entering a swimming pool and avoid swallowing pool water. Take young children for bathroom breaks every 30-60 minutes.
- If you have been diagnosed with Cryptosporidiosis, refrain from swimming for at least 2 weeks following the resolution of your symptoms.
- There is no vaccine to prevent cryptosporidiosis.
Information for Clinicians
Cryptosporidiosis is a ROUTINE/ENTERIC (enteric prevention priority) notifiable condition and must be reported by phone if the individual is a food handler, direct care provider, or pre-school aged child. Otherwise routine reports may be used.
Disease Reporting Phone Numbers (24/7)
Oahu (Disease Investigation Branch): (808) 586-4586
Maui District Health Office: (808) 984-8213
Kauai District Health Office: (808) 241-3563
Big Island District Health Office (Hilo): (808) 933-0912
Big Island District Health Office (Kona): (808) 322-4877
After hours on Oahu: (808) 600-3625
After hours on neighbor islands: (800) 360-2575 (toll free)
For more information: Information for Public Health Professionals on Cryptosporidiosis (CDC)
Last reviewed June 2024