Malaria
About This Disease
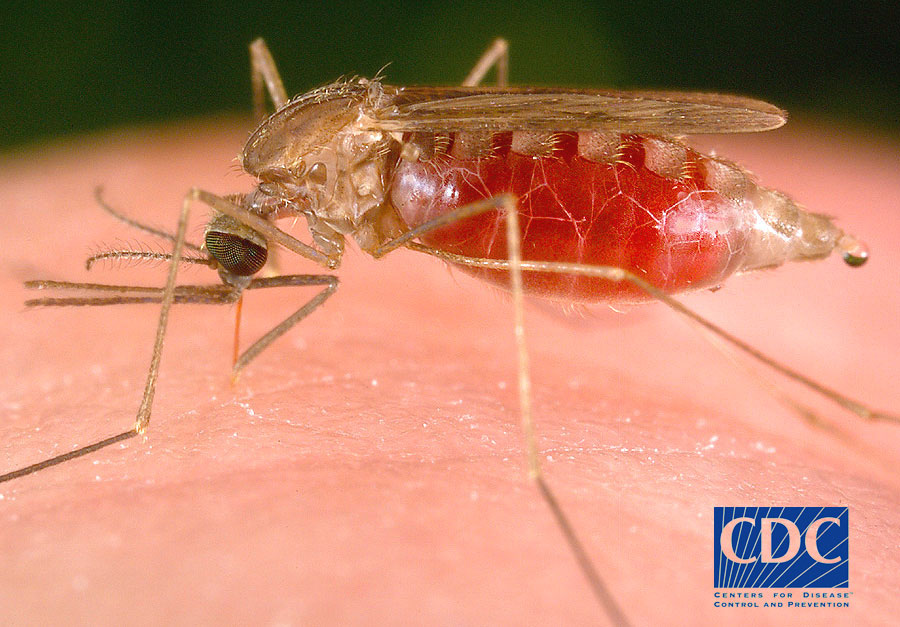
Malaria is a serious mosquito-borne disease caused by parasites in the Plasmodium genus. It is transmitted to humans by the Anopheles mosquitoes. Plasmodium falciparum can cause severe and fatal disease in human. Other members of the Plasmodium genus; P. vivax, P. malariae, P. ovale, and P. knowlesi cause human disease that is generally milder and not life-threatening. Malaria is a significant problem in areas of Asia, Africa, and Central and South America. Unless precautions are taken, any person living in or traveling to a country where malaria is present can get the disease. Malaria is not a problem in Hawaii because the Anopheles mosquito is not found here. However, persons who were infected in malaria endemic regions have been diagnosed with malaria after arrival in Hawaii.
Signs and Symptoms
Symptoms of malaria include fever, chills, backache, and headache. Cycles of chills, fever, and sweating that subside and then return every 1, 2, or 3 days (depending on the type of malaria) are common signs of malaria infection. Malaria can also cause vomiting, diarrhea, coughing, and yellowing (jaundice) of the skin or whites of the eyes. Patients with severe P. falciparum malaria may develop bleeding problems, shock, kidney or liver failure, central nervous system problems, and coma.
The period between the mosquito bite and the start of illness is usually 7 to 21 days. Certain types of malaria parasites can take several months to cause symptoms.
Transmission
Malaria is spread through the bites of infected female Anopheles mosquitoes. When the female mosquito bites, she injects malaria parasites directly into the blood. The parasites then travel through the blood to the liver and infect the red blood cells. Malaria can also be transmitted by blood transfusion, organ transplantation, needle sharing or congenitally from mother to fetus.
Diagnosis
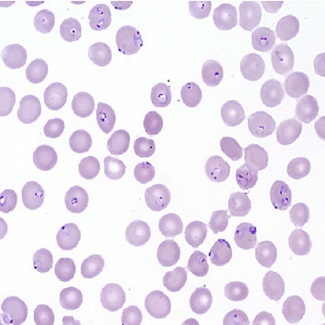
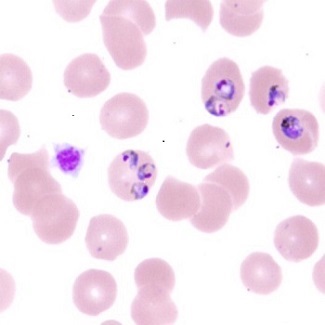
Rapid and acute diagnosis of malaria is integral to providing appropriate treatment and prevention of further spread of infection in the community. Diagnostic laboratory testing can be performed when clinical signs and symptoms are compatible with malaria infection. Both microscopic analysis and nucleic acid detection of the patient’s blood are performed to determine infection.
Treatment
Because different types of malaria have become drug resistant, treatment of malaria infection depends upon the geographic region where a person is infected. Effective medication for each type of malaria must be prescribed by a doctor. As patients infected with P. falciparum malaria can die (often as a result of delayed treatment), immediate treatment is critical. Chloroquine is the drug of choice for acute malaria in sensitive strains.
Risk in Hawaii
Malaria is not a problem in Hawaii because the Anopheles mosquito is not found here. However, persons who were infected overseas have been diagnosed with malaria after arrival in Hawaii.
Prevention
- If you are traveling to an area with risk of malaria, your doctor can prescribe preventive medicines to take. Be sure to take them as directed.
- Avoid exposure to mosquitoes. Wear appropriate clothing such as long-sleeved shirts and long pants especially when outdoors.
- Apply insect repellent to exposed skin or clothing. The recommended repellent contains 20%–35% DEET. Higher concentrations of DEET may have a longer repellent effect, however, concentrations over 50% provide no added protection.
- Use mosquito nets treated with insecticides over beds and screens over windows and doors.
- Spray permethrin or a similar insecticide in the bedroom before going to bed.
If you are planning on traveling, check if there is a risk of malaria at your destination before your trip. Consult with your physician. Depending on the location of travel and risk level, mosquito bite prevention measures with or without chemoprophylaxis may be recommended.
Travel resources: CDC’s Traveler’s Health website and the Malaria Risk Assessment for Travelers page.
Information for Clinicians
Malaria is a reportable disease in the State of Hawaii under the Routine category (Hawaii Administrative Rules Title 11 Chapter 156, Communicable Diseases) The reporting should be made by telephone, fax or mail to the Disease Outbreak Control Division on Oahu or to the District Health Offices on the neighbor islands. A written Communicable Disease Report (CDR) should be submitted by mail or fax.
Last reviewed: July 2019